For many people living with Mast Cell Activation Syndrome (MCAS), the most frustrating part of the condition is how unpredictable symptoms can feel. A meal that seemed safe yesterday may trigger flushing today. Energy levels may feel stable one morning but collapse by afternoon. Skin reactions, headaches, digestive symptoms, or fatigue may appear suddenly without an obvious cause.
This unpredictability can leave patients feeling confused or even doubting their own experience. However, these fluctuations are actually a defining feature of mast cell disorders.
MCAS involves immune cells that respond rapidly to internal and external signals. Because these signals constantly change, symptoms may appear to come and go unexpectedly. Understanding how mast cells work and what triggers them can help explain why symptom patterns vary so widely.
What are Mast Cells and Why Do They Matter?
Mast cells are specialized immune cells found throughout the body. They play a protective role by responding to infection, injury, and allergens.
These cells are especially concentrated in areas where the body interacts with the outside environment, including:
- Skin
- Respiratory tract
- Digestive tract
- Connective tissue
- Blood vessels
When mast cells detect a threat, they release chemical mediators. These include histamine, prostaglandins, cytokines, and leukotrienes.
In normal circumstances, this response helps the body defend itself. In MCAS, however, mast cells may release mediators too readily or too frequently, leading to widespread symptoms.
Why MCAS Symptoms Fluctuate So Much
One reason MCAS feels unpredictable is that mast cells respond to many different signals simultaneously. Triggers can vary day to day, and sometimes even hour to hour.
Below are several categories of factors that may influence mast cell activation.
| Trigger Category | How It May Affect Mast Cells |
|---|---|
| Food triggers | Certain foods may stimulate mediator release |
| Stress | Stress hormones can activate immune signaling |
| Hormonal shifts | Estrogen and other hormones affect mast cell sensitivity |
| Environmental exposures | Chemicals, fragrances, or allergens may trigger reactions |
| Temperature changes | Heat or sudden temperature shifts can activate mast cells |
| Infections | Immune responses may increase mast cell activity |
Because multiple triggers may occur together, symptoms can change quickly.
The “Trigger Load” Concept: Why Symptoms Appear Suddenly
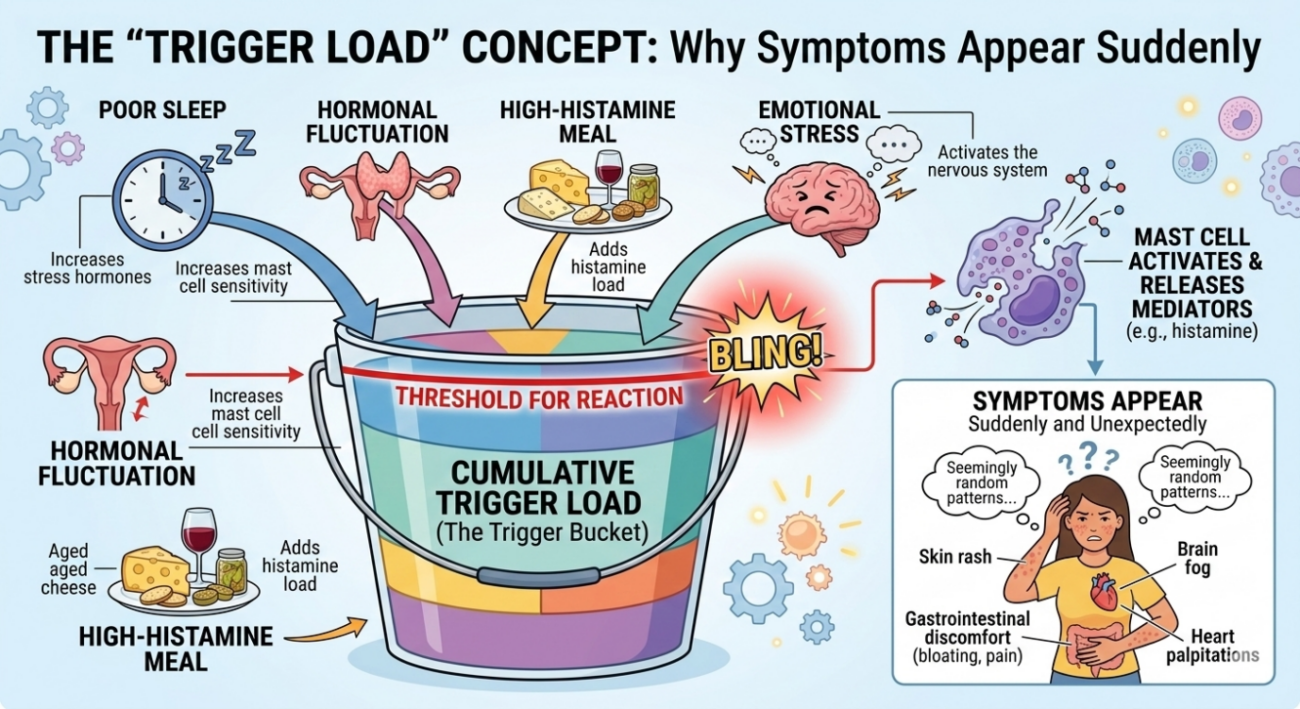
Doctors often explain MCAS symptom patterns using the idea of cumulative trigger load, sometimes called a “trigger bucket.”
Each potential trigger adds to the body’s overall immune stress. When the combined load exceeds a threshold, mast cells release mediators, triggering symptoms.
For example, a person might tolerate one trigger on its own but develop symptoms when several triggers occur together.
Example of Trigger Load
| Possible Trigger | Effect |
|---|---|
| Poor sleep | Increases stress hormones |
| Hormonal fluctuation | Increases mast cell sensitivity |
| High-histamine meal | Adds histamine load |
| Emotional stress | Activates the nervous system |
Individually, these factors may be manageable. Together, they may push mast cells past a threshold for a reaction.
Understanding this cumulative effect can help patients recognize patterns that initially seem random.
Histamine Metabolism: Why Some People React More Easily
Another reason symptoms fluctuate involves how the body processes histamine.
Two important enzymes help break down histamine:
| Enzyme | Role |
|---|---|
| DAO (Diamine Oxidase) | Breaks down histamine in the digestive tract |
| HNMT (Histamine-N-Methyltransferase) | Breaks down histamine inside cells |
If these enzymes are reduced or overwhelmed, histamine may accumulate in the body. This can increase the likelihood of symptoms such as flushing, headaches, digestive discomfort, or skin reactions.
Factors that influence histamine metabolism may include genetics, gut health, and nutritional status.
PRO TIP
Some individuals notice symptom improvement when they support overall digestive health and avoid large amounts of high-histamine foods during periods of increased sensitivity.
The Gut–Mast Cell Connection
The digestive system contains one of the highest concentrations of mast cells in the body.
These immune cells play an important role in regulating gut barrier function and protecting against pathogens. However, when mast cells become overactive, digestive symptoms may occur.
Common gastrointestinal symptoms in MCAS may include:
- Bloating
- Abdominal discomfort
- Reflux
- Diarrhea or constipation
- Food sensitivities
Gut inflammation, microbiome imbalance, or infection may further increase mast cell activity.
Because of this relationship, digestive health often plays an important role in managing mast cell conditions.
The Nervous System and Mast Cells
The immune and nervous systems constantly communicate.
Mast cells are located near nerve endings throughout the body. When mast cells release mediators, they can stimulate nearby nerves. At the same time, nerve signals can also activate mast cells.
This creates a feedback loop where nervous system stress may increase mast cell activation, and mast cell mediators may increase nervous system sensitivity.
This interaction helps explain symptoms such as:
- Headaches
- Temperature sensitivity
- Fatigue
- Anxiety-like sensations
Managing nervous system stress may therefore help reduce mast cell reactivity for some individuals.
Hormones and Mast Cell Activity
Hormones influence immune signaling throughout the body.
Many individuals with MCAS notice symptom patterns during hormonal changes, such as:
- Menstrual cycles
- Pregnancy
- Perimenopause
Estrogen in particular can influence mast cell activation. As hormone levels fluctuate, mast cells may become more sensitive to triggers.
Tracking symptoms alongside hormonal cycles can sometimes reveal patterns that help guide lifestyle adjustments.
Environmental and Medication Sensitivities
Individuals with mast cell disorders may also react to environmental exposures or medications.
Possible triggers may include:
- Fragrances or perfumes
- Cleaning chemicals
- Smoke or pollution
- Alcohol
- Certain medications such as NSAIDs or antibiotics
Not everyone reacts to the same triggers. Identifying individual sensitivities can help reduce unexpected symptom flares.
Conditions That Often Overlap With MCAS
MCAS frequently occurs alongside other conditions that affect immune or connective tissue regulation.
Some commonly associated conditions include:
- Dysautonomia or POTS
- Ehlers-Danlos Syndrome
- Chronic fatigue conditions
- Gastrointestinal motility disorders
These overlaps may contribute to complex symptom patterns and highlight the importance of evaluating the body as a whole.
A Whole-Body Perspective on Mast Cell Health
Because mast cells interact with multiple systems, management often focuses on improving overall physiological stability rather than targeting a single symptom.
At Byhartz, Dr. Cara Hartz works with individuals seeking MCAS treatment in Seattle who want a thoughtful and personalized approach to immune and nervous system balance.
Care may involve evaluating patterns related to:
- Immune activation
- Digestive health
- Nervous system regulation
- Environmental triggers
- Lifestyle factors that influence inflammation
Plans are individualized and adjusted based on each person’s symptoms and goals.
PRO TIP
Keeping a symptom journal that tracks food intake, stress levels, sleep patterns, and environmental exposures can help identify triggers that may not be immediately obvious.
Important Points to Remember About MCAS
- Mast cells are part of the body’s normal immune defense system.
- In MCAS, these cells may release mediators more easily than expected.
- Symptoms can fluctuate because mast cells respond to multiple triggers.
- Individual trigger patterns vary widely between patients.
- Gradual stabilization is often more effective than aggressive self-treatment.
A Note of Caution About Self-Treating MCAS
Information about mast cell disorders has expanded rapidly online, but not every strategy is appropriate for every individual.
Highly restrictive diets or aggressive supplement regimens without professional guidance may lead to unintended complications such as nutrient deficiencies or worsening sensitivities.
If symptoms persist or are severe, consulting a qualified healthcare professional can help ensure safe and appropriate care.
Frequently Asked Questions
Why do MCAS symptoms feel random?
Symptoms often appear random because mast cells respond to multiple triggers simultaneously. When several triggers occur together, symptoms may appear suddenly.
Can stress worsen mast cell symptoms?
Yes. Stress hormones can influence immune signaling and may increase mast cell reactivity.
Is MCAS the same as an allergy?
No. MCAS involves abnormal mast cell mediator release without the typical allergy antibody response.
Do all patients react to the same triggers?
No. Triggers vary widely between individuals.
Can symptoms improve over time?
Many individuals experience improved stability when triggers are identified and supportive management strategies are implemented.
Conclusion
Mast Cell Activation Syndrome can feel unpredictable, but symptoms rarely occur without underlying patterns. Mast cells respond to many signals, including stress, hormones, environmental exposures, and digestive health, which explains why symptoms may fluctuate.
By understanding how these systems interact, patients can begin to recognize triggers and develop strategies that support greater stability.
With thoughtful care and individualized support, many people living with mast cell disorders are able to improve symptom management and regain a greater sense of control over their health.

