For many people living with Postural Orthostatic Tachycardia Syndrome (POTS), one of the most confusing aspects of the condition is how unpredictable the symptoms can be.
Some days may feel manageable, while on other days even simple activities-standing up, walking across a room, or taking a shower – can trigger dizziness, fatigue, or a racing heart.
This fluctuation can make patients question what is happening in their bodies. However, this variability is actually one of the defining characteristics of autonomic nervous system disorders.
POTS is not simply a heart rate issue. It is a condition involving autonomic nervous system regulation, which means symptoms can change depending on how the nervous system responds to stress, circulation demands, hydration levels, hormones, and environmental conditions.
Understanding the physiology behind these changes can help patients make sense of their symptoms and identify strategies that support greater stability.
Understand the Autonomic Nervous System
The autonomic nervous system controls the body’s automatic functions. These are processes that happen without conscious effort.
Examples include:
- heart rate regulation
- blood pressure control
- circulation
- digestion
- body temperature regulation
- stress response
This system has two primary branches that constantly balance one another.
| Nervous System Branch | Primary Role |
|---|---|
| Sympathetic Nervous System | Activates the body during stress (“fight or flight”) |
| Parasympathetic Nervous System | Promotes recovery and restoration (“rest and digest”) |
In people with dysautonomia, this balance becomes disrupted.
When the body attempts to adapt to everyday changes, such as standing, heat, or stress, the nervous system may respond in exaggerated or inefficient ways.
What Happens in the Body When Someone with POTS Stands Up
To understand why symptoms fluctuate, it helps to look at what happens physiologically when a person changes posture.
Step-by-Step Nervous System Response
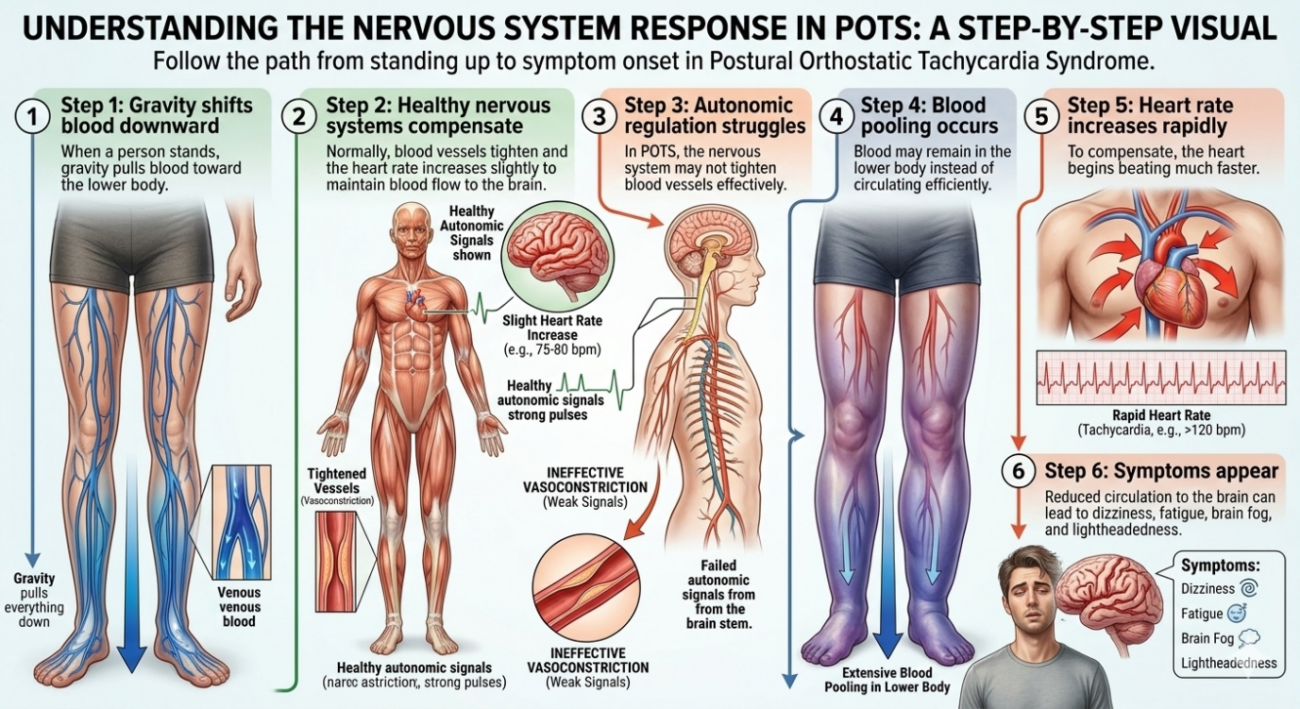
Step 1: Gravity shifts blood downward
When a person stands, gravity pulls blood toward the lower body.
Step 2: Healthy nervous systems compensate
Normally, blood vessels tighten and the heart rate increases slightly to maintain blood flow to the brain.
Step 3: Autonomic regulation struggles
In POTS, the nervous system may not tighten blood vessels effectively.
Step 4: Blood pooling occurs
Blood may remain in the lower body instead of circulating efficiently.
Step 5: Heart rate increases rapidly
To compensate, the heart begins beating much faster.
Step 6: Symptoms appear
Reduced circulation to the brain can lead to dizziness, fatigue, brain fog, and lightheadedness.
Why Symptoms Can Change from Day to Day
The autonomic nervous system responds to many internal signals. Because these signals vary daily, symptom severity may also change.
Below are some of the most common factors that influence POTS symptoms.
| Factor | Why It Matters |
|---|---|
| Hydration levels | Low blood volume worsens circulation instability |
| Sleep quality | Poor sleep increases nervous system stress |
| Hormonal changes | Hormones affect vascular tone and circulation |
| Stress levels | Stress activates the sympathetic nervous system |
| Temperature | Heat dilates blood vessels and increases pooling |
| Illness or inflammation | Immune activity can disrupt autonomic balance |
Even small changes in these areas may influence how someone feels on a given day.
The Role of Blood Volume in POTS
Many individuals with POTS have a lower-than-expected circulating blood volume.
This means there is simply less fluid available to maintain stable circulation when standing.
When blood volume is low, the body must work harder to move blood back to the heart and brain.
This often results in:
- rapid heart rate
- fatigue
- dizziness
- exercise intolerance
Increasing hydration and supporting circulation can sometimes improve symptom stability.
PRO TIP
Many patients notice symptom improvement when they consistently focus on hydration, electrolyte balance, and gradual physical conditioning. These simple habits can help support circulation and nervous system stability over time.
Hormones and POTS Symptom Fluctuations
Hormonal changes can influence blood vessel function and nervous system regulation.
Some individuals notice symptom changes during:
- menstrual cycles
- pregnancy
- perimenopause
- periods of hormonal imbalance
Hormones affect vascular tone, which can influence how easily blood vessels tighten when standing.
This is one reason symptoms may feel worse at certain times of the month.
Why Heat and Temperature Make Symptoms Worse
Many people with POTS feel significantly worse in warm environments.
Heat causes blood vessels to dilate. When vessels widen, blood is more likely to pool in the lower body.
This can reduce blood flow to the brain, leading to symptoms such as dizziness or fatigue.
Hot showers, warm weather, and poorly ventilated environments may therefore trigger symptom flares.
Conditions That Often Overlap With POTS
POTS frequently occurs alongside other conditions affecting connective tissue, immunity, or metabolism.
Some commonly associated conditions include:
- Ehlers-Danlos Syndrome
- mast cell activation syndrome (MCAS)
- chronic fatigue conditions
- gastrointestinal motility disorders
Understanding these overlaps can help clinicians identify broader patterns affecting nervous system regulation.
A Whole-Body Approach to Dysautonomia Care
Because POTS involves multiple systems, treatment often focuses on improving overall physiological stability rather than targeting only heart rate.
At Byhartz, Dr. Cara Hartz works with patients seeking a specialist doctor for POTS and dysautonomia naturopath in Seattle who understands how circulation, metabolism, and nervous system balance interact.
Care may include strategies aimed at supporting:
- nervous system regulation
- circulation stability
- hydration and electrolyte balance
- metabolic health
- digestive function
Each plan is tailored to a patient’s symptoms and lifestyle.
PRO TIP
Tracking patterns such as hydration, sleep, activity, and stress can help patients identify triggers and anticipate symptom fluctuations.
Important Points to Remember About POTS
• POTS symptoms fluctuate because the autonomic nervous system responds to many internal and external factors.
• Hydration, sleep, hormones, and stress can significantly influence symptom severity.
• Dysautonomia often overlaps with other medical conditions.
• Personalized management strategies can improve long-term stability.
A Note of Caution About Self-Managing POTS
Online information about POTS is widely available, but not every recommendation is appropriate for every patient.
Aggressive exercise programs, restrictive diets, or excessive supplementation without professional guidance may worsen symptoms in some individuals.
If symptoms interfere with daily functioning, consulting a qualified healthcare professional can help ensure that management strategies are safe and appropriate.
Frequently Asked Questions
Why do POTS symptoms change daily?
The autonomic nervous system responds to hydration, hormones, sleep quality, stress, and environmental factors.
Is POTS dangerous?
For most individuals, POTS is not life-threatening, but symptoms can significantly affect quality of life.
Can stress worsen POTS symptoms?
Yes. Stress activates the sympathetic nervous system and may intensify symptoms such as tachycardia and fatigue.
Can POTS improve over time?
Some individuals experience improvement with appropriate management strategies and lifestyle adjustments.
Conclusion
Living with POTS can feel unpredictable, but the fluctuations many patients experience are often linked to how the autonomic nervous system responds to daily stressors.
By understanding the underlying physiology, patients can begin to identify patterns and adopt strategies that support greater stability.
With thoughtful care and individualized support, many people living with dysautonomia are able to improve their quality of life and regain confidence in their daily activities.

